Low Back Pain
Back pain isn’t usually a sign of a serious medical condition – it’s more likely a muscle strain or a ligament sprain - and often there is no particular cause..
Back pain is sometimes linked with pain in one or both legs (sciatica), muscle weakness, numbness and tingling in the legs + fee - due to irritation of the spinal nerve roots.
If you lose bladder or bowel control you should see your doctor urgently.
With persistent LBP the lack of movement can cause muscle weakness + joint stiffness. It’s important that you keep moving as much as possible.
Physiotherapy can help with acute and chronic back pain.
Chartered Physiotherapists can provide a variety of treatments such as
1. Manipulation,
2. Massage,
3. Electrotherapy,
4. Functional Rehabilitation exercises,
5. Advice on
-
The cause of your problem
-
Return to your normal activities
-
Prevention of pain returning in the future.
Exercise is the most important way that you can:
-
ease stiffness and pain
-
build up muscle strength and stamina
-
improve your flexibility and general fitness.
These benefits continue for some weeks after the pain and symptoms subside so it is advisable to persist with the exercises for a period after the pain has gone.
Consult Ennis Physiotherapy Clinic if you need an assessment, treatment or advice


Neck Pain
Most people will have neck pain during their life. It may not be possible to identify the exact cause. ‘Age related’ wear + tear and poor posture are often observed. The severity of symptoms may vary
.
If you have
1. Severe pain in the neck
2. Pain in the shoulder and/or shoulder blade area or
3. Pain down into the arm(s)
then you need assessment and treatment by a chartered physiotherapist.
Remaining active and physiotherapy can accelerate your recovery.
‘Whiplash’ occur when a sudden movement of the head and neck injure the ligament and muscle of the neck area, This may cause pain, stiffness and reduced movement / activity. There may be other signs + symptoms in the head, neck, shoulders and arms
The duration of neck pain is very variable.
Headache can be caused by sprain / strains of the upper neck area. This responds well to manual and exercise therapy provided by Chartered Physiotherapists.
Contact the clinic for assessment and treatment of neck, head, shoulder or arm pain.


Neck Care Advice
1. Maintain good posture and alignment of the head and neck.
-
Avoid excessive flexed or slouched positions.
-
Stand or sit tall with the shoulders relaxed,
-
The head in line with the body / keep the ears over the shoulders..
2. Avoid Prolonged Sitting
3. Sit with good spinal and especially lumber support
4. Ensure computer workstations are correctly set up
5. Tilt reading material up towards you.
6. Consider using 'hands free' if you spend long periods on the phone.
7. Do not hold a phone between your ear and your shoulder
8. Do not slouch while driving – position the seat to support you correctly.
9. Sleeping
-
Avoid sleeping on your stomach
-
Sleep on the back in preference to on the side if possible
-
Support the neck only with pillows for good alignment of the head + neck – do not have it sagging to side, twisted or excessively flexed.
d. One pillow is usually sufficient if lying on the back and two if on the side.
-
Pillows should not be under the shoulder - only under the head + neck.
10. Avoid prolonged static postures – take regular breaks.
11. Avoid excessive amounts of looking or reaching upwards
-
use a steps / ladder to raise yourself so there is not a need to work above shoulder height.
12. Avoid carrying loads on one side.
-
Spread the pressure more evenly by using both shoulder straps on a bag.
-
supporting the load from underneath using both hands.
Consult Ennis Physiotherapy Clinic if you need assessment, treatment or advice about your neck pain,.

Posture and Spinal Pain
Postural strain is a common factor and cause of spinal discomfort.
‘Normal’ posture develops during childhood and young children generally have good posture.
Poor postural habits can occur at any time but generally become habitual during or after teenage years.
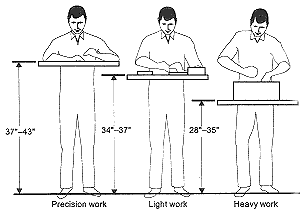
The selection of age appropriate furniture (height / size) for work, or leisure, is crucial for encouraging good posture . However even the best ergonomic furniture can be used badly and is no guarantee of good posture. For example even with an appropriate chair a person may sit poorly. If the seat is too low or too deep the pelvis will tilt backwards and the spine must flex - this puts pressure on the discs, joints and ligaments.
Good posture can be achieved when the eyes are held level and facing forward, the shoulders are level, the pelvis is held in neutral and where there is relative muscle balance around the pelvis and shoulder girdle areas.
For more detailed information relating to posture please see the posture page


Intervertebral Disc
Injury pf the Intervertebral discs is a well known risk factor for spinal pain.
Unfortunately there are many theories of how and why the discs are so commonly involved in spinal pain. A whole range of terminology has entered normal usage which facilitates and perpetuates this poor understanding of the disc
.
The disc can be injured in a number of ways. The pain associated with disc injury is rarely from the disc itself but more likely from other tissues affected by the disc injury.
The disc consists of a laminated cartilage wall (Annulus) which encloses a gel like liquid (the Nucleus). The nucleus attracts water very strongly and draws fluid into the disc when lying down - increasing the pressure within the disc i.e. in the morning. When up and moving this fluid is slowly squeezed out again. This movement of fluid helps supply the disc with nutrition so movement is important. Over a lifetime the fluid content of the nucleus is gradually lost, and it becomes more solid with ageing. The wall of the disc is attached to the vertebra bone above + below it, and is completely enclosed all around by strong spinal ligaments. Thus the disc is not free to move i.e. it does not “ go in or out”
.
The laminations of the disc wall allow the bones of the spine to bend and rotate a little bit relative to each other - the bones + ligaments keep this movement limited. Total movement is produced by a little movement occurring at each of a number of segments at the same time.
The lower level discs are larger as they carry more weight - the lumber discs are the biggest.
There is minimal blood + nerve supply to the discs and so they are slow to heal and healthy discs do not generally generate pain.
Over years the laminations of the disc wall become separated, weakened and begin to crack.
As the spine is loaded (poor postures / lift poorly) the nucleus is forced into the cracks and very gradually can deepen + widen the cracks. The disc wall gradually weakens and
may begin to bulge - similar to a soft tyre - and it may even ‘blister’ in a localised bulge. .
Such a disc is very vulnerable and prone to further serious injury, especially from sudden, pressure within the disc (caused by rapid bending movements, falls,
jerking, coughing etc) that can cause the bulge to ‘burst’ or crack open, and the nucleus material is free to ooze to the outside of the disc.- a so called ‘slipped disc’, ‘putting the disc out’, ‘bursting the disc’ - which is called a Prolapsed disc (in medical terminology).
As the nuclear material reaches the outside of the disc it attracts + absorbs water strongly causing it to expand rapidly in size. This can put pressure on the surrounding tissues which may be pain sensitive, such as nerve roots.
Unfortunately in humans the weakest part of the disc wall is next to spinal nerve root is exiting from the spine. Pressure on this nerve is likely to provoke pain and other symptoms.
A disc that has repeatedly been injured over years is likely to appear thinner on x-ray, often then called a worn disc’. These discs do not maintain the normal separation between the vertebral bones and hence the joints of the spine at that level are likely to wear or degenerate / become arthritic more quickly than would otherwise be the case.


Treatment of Spinal + Discal Injury
ITreatment minimises the impact of the injury on surrounding tissues and to the disc itself. Management of pain and resting normal movement in the spine are the key goals.
A combination of treatment modalities is used to achieve them. Rest + avoiding things that aggravate the pain is recommended in the first week.
-
Medication and heat / cold packs are recommended for pain symptoms.
-
Avoid / minimise sitting down if possible - especially in low seating.
-
Keep good postures when sitting or standing
-
Avoid prolonged periods in any one posture. See here for posture info.
-
Avoid prolonged periods in bedrest beyond 1-2 days.
-
Begin exercise ASAP - don’t wait for pain to get bad!!
-
Remain as active as possible - it is by doing so that your back will get strong.
-
Be proactive in preventing and protecting your discs.
-
Apply good ergonomics when selecting furniture, cars, at work + at leisure.
-
Strengthen your back when the injury is resolved and regain core stability. Pilates and yoga can help - no one approach suits everyone.
Exercise programmes need to combine flexibility, strength training and functional activities appropriate for ones needs.
A good attitude to protecting your discs - it is not what you do so much as how you do it! An injured disc can recover and can become strong again. Your spine must become ‘fit’ for what it needs to be able to do each day and it must be protected and cared for - but not too much so..
This exercise helps regain flexion in a safe way for the disc. Lying down minimises the pressure within the disc. The flexion will raise it slightly while allowing the joints of the spinal column to be stretched. Other exercises while lying down include some rotation of the trunk or those done in prone (on tummy) or in kneeling.
The best exercise programmes will include a mix of stretching, strengthening and functional exercises. The latter will reflect the movements + activity encountered daily. They may be incorporated into activities such as walking or running. Core stability, pilates + yoga may fall into this category.





